Disclosure :: This post is sponsored by Ochsner Health.
5 Reasons to Get A Mammogram Before Age 40
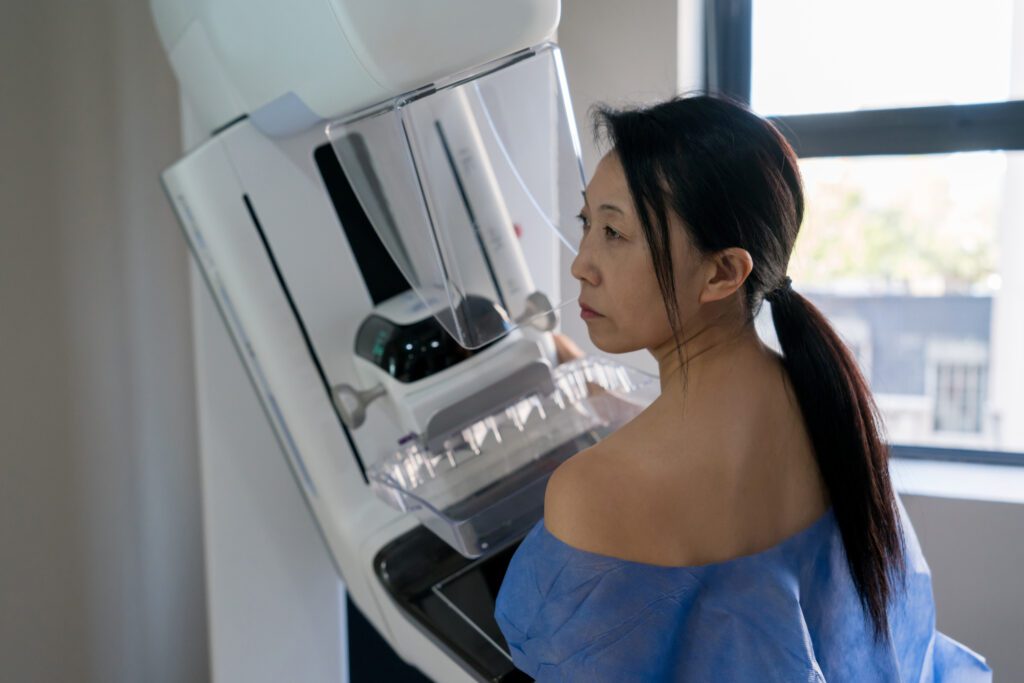
A general guideline for routine cancer screenings is that mammograms are recommended annually for women beginning at the age of 40. But everyone is unique, and depending on various factors, you may need to start getting mammograms before you turn 40. In fact, some women may need to begin getting mammograms in their 20s or 30s. Here are five reasons to get screened for cancer before 40.
- Your family history. If you have relatives who have had breast cancer or other cancers, screening is recommended to begin at 25 years old or 10 years before the age of the earliest affected relative in your family. If you don’t know your family history, start having these important conversations with your family members now. If you are younger and you’re experiencing symptoms of breast cancer without a prior family history, talk to a healthcare professional about your concerns.
- A genetic mutation. The presence of genetic mutations, including BRCA1 and BRCA 2 will make you a higher risk for breast cancer. The National Cancer Institute states, “BRCA1 (BReast CAncer gene 1) and BRCA2 (BReast CAncer gene 2) are genes that produce proteins that help repair damaged DNA. Everyone has two copies of each of these genes—one copy inherited from each parent. BRCA1 and BRCA2 are sometimes called tumor suppressor genes because when they have certain changes, called harmful (or pathogenic) variants (or mutations), cancer can develop.” Genetic testing would be required to determine if you have these genetic mutations, and if you do, your doctor will recommend that you get screened early.
- Your race/ethnicity. Data shows that white women are more likely to develop breast cancer than Black, Hispanic and Asian women. Black women are more likely to develop more aggressive, more advanced-stage breast cancer that is diagnosed at a young age. According to the CDC, Black women die from breast cancer at a higher rate than white women. American College of Radiology recommends that Black women have a risk assessment at age 30 to see if earlier screening is needed. Women of Ashkenazi Jewish descent are also at significantly higher risk for breast cancer. The CDC states that 1 in 40 Ashkenazi Jewish women has a BRCA gene mutation. It is important to talk with your doctor about your personal risk factors.
- If you’ve been exposed to radiation. If your chest has been exposed to radiation between age 10 and 30, you may need early breast cancer screenings. One reason your chest may have been exposed to radiation would be through radiation therapy. Consult your doctor.
- If you have dense breasts. Women with higher breast density have a greater risk of getting breast cancer. Breasts have three kinds of tissue: fibrous tissue holds the breast tissue in place. Glandular tissue is the part of the breast structure that makes milk. And fatty tissue gives the breast their size and shape. Breast density is the amount of fibrous and glandular tissue in a woman’s breast compared to the amount of fatty tissue. Breast density is determined on a mammography report based on a variety of factors, and it is important for women to know their breast density because women with dense breasts have a higher chance of getting breast cancer, though the reason behind this is unclear. Dense breast tissue can hide cancers, and women with dense breasts may need additional testing beyond a mammogram, including an ultrasound of the breasts and an MRI. Those who are most likely to have dense breasts include young women, pregnant/breastfeeding women, those taking hormone replacement therapy and those who have a lower body weight percentage.
Mammograms and Breast Cancer Symptoms
If you’ve never had a mammogram before, here’s what to expect. A mammogram is an X-ray of the breast. This procedure is currently the best way to detect breast cancer earlier when it is easier to treat. The typical length for a screening, including the mammogram, is about 15-20 minutes. The pressure from a mammogram is like that of a blood pressure cuff. During the exam, your technologist will position your breast within the mammography unit and carefully apply compression. Compression improves the quality and accuracy of your images. Your exam will be performed by a specially trained technologist in a private room, who will also ask specific questions to assess each patient’s individual breast cancer risk. The questions range from the age of your first period, height, weight, childbearing history, menopause status, hormone replacement therapy and family history of breast or ovarian cancer. After your screening mammogram, a radiologist will review your images and issue a report. Results are available through your MyOchsner portal and by mail within a few days.
No matter your age, you should practice breast awareness. Be aware of changes in your breast and continue to perform at-home breast exams. Some common symptoms of breast cancer include the following:
- New lump in the breast or underarm (armpit)
- Extreme breast tenderness
- Thickening or swelling of part of the breast
- Irritation or dimpling of breast skin
- Redness or flaky skin in the nipple area or the breast
- Pulling in of the nipple or pain in the nipple area
- Nipple discharge other than breast milk, including blood
- Any change in the size or the shape of the breast
- Pain in any area of the breast
- Burning sensation in any part of the breast
- Scarring, rashes or moles that were not there before
If you feel like something has changed, you should see a healthcare provider as soon as possible.
To learn more about cancer screenings at Ochsner Health, visit ochsner.org/cancer-screenings.
About the author





















