Disclaimer: This is a guest post from Dr. Leanne Redman, associate professor of women’s health studies at Pennington Biomedical Research Center. You can get to know her more here and read her first post here. Her facts and opinions are based on her personal research. Red Stick Moms Blog was not paid to promote any specific medical viewpoints or studies. Always consult your physician with any medical questions.
January is “National Cervical Health Awareness” month. The World Health Organization reports cervical cancer as the second most common cancer in women. BUT did you know cervical cancer is now one of the most preventable cancers women are diagnosed with? It is estimated that in 2015, nearly 13,000 women will be diagnosed with cervical cancer and these diagnoses could be prevented! I wanted to chat this month about cervical cancer- what it is, how you can be tested for it, and how you can prevent it.
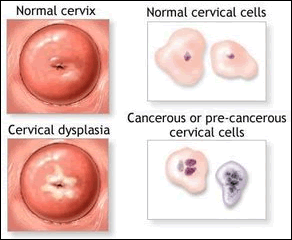
Cervical cancer is a condition that occurs when cancerous cells develop on the cervix. One characteristic of a cancerous cell is that they keep growing and multiplying out of control resulting in a tumor. Before becoming “full blown” cancer, normal cells on the cervix transform into precancerous cells. If caught early (meaning when cells are in the precancerous stage), we have a better chance of preventing the precancerous cells from becoming cancer. Transformation of precancerous cells into cancerous cells usually occurs over several years, but may happen in less than a year if not caught early, so it is important to continue to monitor your cervical health.
What are the risk factors for cervical cancer?
One of the most significant risk factors that can increase your likelihood of developing cervical cancer is a human papilloma virus (HPV) infection. HPV is a very common sexually transmitted infection. At least 50% of people who have been sexually active will contract HPV at some point in their lives. HPV can infect cervical cells and cause genital warts, however some people with HPV may never develop symptoms making testing that much more important.
Other risk factors that increase a woman’s chances for cervical cancer are smoking, long term use of contraceptives, giving birth to 3 or more children, having several sexual partners, and a family history of cervical cancer. Even as adults, discussing sexual habits, sexual history, and other lifestyle factors with a health care provider can be uncomfortable. It is likely even more embarrassing for our children to discuss these topics. If you or your child is sexually active, whether it is with one partner or multiple partners, cervical screening is vital to the detection and protection against cervical cancer and can literally save a life. It is important to develop a safe, open, and honest relationship with your provider so that he or she can provide the best care possible for you and your family.
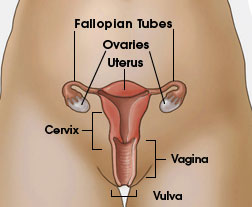

The first step to fighting cervical cancer is detecting and identifying cancerous and precancerous cells through screening tests, such as Pap Smears and Human Papilloma Virus (HPV) tests.
1) A Pap Smear is a procedure which collects some cells from the cervix and examines them under a microscope looking for cancerous or precancerous cells (which look different than normal cells). To collect these cells, physicians or midwives brush the cervix with an instrument that collects these cells for analysis.
2) The HPV test uses the same procedure as the Pap Smear to collect cells for testing, so testing for HPV at the same time as having a Pap Smear can easily be done (this is called co-testing). Screenings, both Pap Smears and HPV, can be done at the same time as pelvic exams, but are not required for pelvic exams.
So when should screening for cervical cancer begin?
The American College of Obstetricians and Gynecologists (ACOG) have compiled a cervical cancer screening patient education fact sheet to communicate the current screening recommendations.
1) Cervical cancer screenings are recommended for women aged 21 years and older.
2) Previously, pap smears were suggested annually, but with recent scientific evidence, most women only need a pap smear every 3 years. This scientific evidence shows that annual screenings or too frequent screenings can cause more harm than benefit. False positive results are relatively common with frequent cervical cancer screenings, and invasive follow up procedures for these test results can have negative side effects, including problems related to future pregnancies, delivery complications, or anxiety.
3) As of 2012, in accordance with the ACOG guidelines, the American Cancer Society and US Preventive Services Task Force recommend co-testing (both Pap and HPV testing) every 5 years for women aged 30 to 65 years. HPV testing is not generally recommended for women under the age of 30.

Isn’t there a vaccination for HPV?
Yes. Vaccinations against HPV can also be used as a line of defense to protect against cervical cancer and other cancers caused by HPV in both men and women. In the United States, approximately 17,500 women and 9,300 men are infected with cancers caused by HPV each year. Gardasil® and Cervarix® are types of HPV vaccinations available which can prevent HPV infection. These vaccinations are given in a series of 3 shots within 6 months for girls and boys, generally at 11 or 12 to 26 years of age for women and 21 for men. Once the series of shots is complete, no booster doses are required for the vaccination, and the vaccine lasts in the body for at least 10 years without losing its effectiveness. Studies have been completed in Australia where there is a high prevalence of HPV vaccination usage and have found that HPV vaccination significantly decreases genital warts and the incidence of cervical precancerous cells and abnormal Pap Smear results.
But is the vaccine safe for me and/or my child?
The vaccines have gone through years of extensive safety testing before being made available to the public by the Food and Drug Administration (FDA). The safety and long-term efficacy of the vaccines continues to be monitored and researched. There are no serious safety concerns associated with the vaccines. The vaccines may cause mild to moderate side effects that do not last long and resolve on their own which may include, but are not limited to, pain or redness/swelling at injection site, fever, headache, or feelings of light headedness.
The Centers for Disease Control and Prevention (CDC) created a HPV Infection Fact Sheet for the Public that may help with any additional questions and concerns about the HPV vaccine and HPV infection. You can always discuss the vaccination with your physician or your child’s pediatrician as well. Cervical cancer screenings and HPV vaccinations are covered by most insurance providers. If your insurance does not cover this vaccination for your child, the Vaccines for Children (VFC) program may be able to help. It is recommended that vaccinated women and girls of recommended screening age continue regular screenings for cervical cancer.























